Is It Normal for My Gums to Bleed Every Time I Floss?

Is It Normal for My Gums to Bleed Every Time I Floss?
The Question Half of All Dental Patients Are Thinking
Most people who floss regularly — or who have recently started flossing after a gap — will have noticed some bleeding at the gumline. And most of them have quietly filed this away under ‘probably fine’ and carried on. A few have stopped flossing altogether because of it, reasoning that if flossing makes things bleed, perhaps it is best to leave well enough alone.
Here is what a dentist would tell you in the chair: bleeding gums when flossing is common, but it is not normal. The distinction matters. Common means many people experience it. Normal means it is how healthy gum tissue behaves. Healthy gums do not bleed when you floss — and when they do bleed, it is the gum tissue telling you something worth listening to.
That said, the cause is not always serious, the fix is often straightforward, and understanding what is actually happening is the first step to doing something useful about it. This blog covers exactly that — in plain language, the way a dentist would explain it to a patient sitting in front of them.
🔑 Key Takeaways
- Healthy gum tissue does not bleed during flossing. Bleeding is a sign of inflammation, not a sign that you are flossing too hard.
- The most common cause of gums bleeding when flossing is gingivitis — early-stage gum disease caused by plaque buildup at the gumline.
- Gingivitis is reversible. With improved oral hygiene and a professional clean, most patients see a significant reduction in bleeding within two to four weeks.
- Stopping flossing because of bleeding is the worst response — it allows the plaque causing the inflammation to continue accumulating.
- Bleeding that persists despite good oral hygiene, or that is accompanied by swelling, recession, or sensitivity, warrants a dental assessment.
- Gum disease is the leading cause of tooth loss in adults worldwide — and it begins silently, with bleeding gums as one of the earliest visible signs.
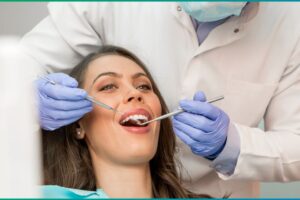
What Healthy Gums Actually Look Like — and Feel Like
Before we talk about what causes bleeding, it helps to know what you are comparing against. Healthy gum tissue has a distinct set of characteristics that most people have never been explicitly told to look for.
Healthy gums are:
- Pink and firm — not red, swollen, or puffy. The colour should be an even, pale pink across the gumline, darker in pigmented individuals but consistent in tone.
- Tightly adapted to the tooth surface — gum tissue should fit snugly around each tooth without gaps, puffiness, or pulling away from the crown.
- Not tender to touch — pressing on healthy gum tissue should not cause discomfort or pain.
- Non-bleeding — healthy gums do not bleed when you floss, when a dentist probes them with an instrument, or when you brush firmly.
- Not receding — the gumline should sit at a consistent level around each tooth, not revealing root surface below the enamel.
If your gums bleed when you floss, they are inflamed — which means the blood vessels within the gum tissue have become engorged and fragile in response to bacterial irritation. The inflammation is the body’s immune response to the presence of plaque and the bacteria it contains. It is not a coincidence, it is not bad luck, and it is not caused by flossing too hard. It is a signal.
Why Gums Bleed When You Floss: The Actual Causes
Gingivitis — The Most Common Reason
Gingivitis is inflammation of the gum tissue caused by the accumulation of bacterial plaque at and just below the gumline. It is the most common cause of gums bleeding when flossing, and it is extremely prevalent — estimates suggest that more than 80% of Indian adults have some degree of gingivitis at any given time.
Plaque is a sticky, colourless film of bacteria that forms on tooth surfaces within hours of brushing. When plaque is not removed through regular brushing and flossing, it remains at the gumline and triggers an inflammatory response in the adjacent gum tissue. The gums become red, swollen, and fragile — and bleed easily when disturbed by floss, a toothbrush, or a dental instrument.
The important thing to understand about gingivitis is that it is entirely reversible. There is no permanent damage to the bone or supporting structures of the tooth at this stage. Improved oral hygiene — and in most cases a professional scale and polish to remove the hardened tartar that brushing alone cannot shift — resolves gingivitis and stops the bleeding. Most patients who commit to consistent flossing and cleaning see a noticeable reduction in bleeding within two to four weeks.
Tartar Buildup
Plaque that is not removed within 24 to 72 hours hardens into tartar — also called calculus — a mineralised deposit that adheres firmly to the tooth surface and cannot be removed by brushing or flossing at home. Tartar is a continuous irritant to the gum tissue, sustaining and worsening the inflammatory response even in patients who are otherwise brushing and flossing correctly.
This is why a professional dental clean is an essential component of gum disease management — not just a cosmetic polish, but the removal of the hardened deposits that maintain the inflammatory cycle. Flossing alone cannot remove tartar once it has formed. Only an ultrasonic scaler or hand instruments used by a dental professional can do this.
Infrequent or New Flossing
If you floss occasionally rather than daily, or if you have recently restarted flossing after a long gap, bleeding is expected — because the gum tissue around the contact points between teeth is likely already inflamed from plaque accumulation in those areas. Flossing disturbs the inflamed tissue, causing temporary bleeding.
This is not a reason to stop flossing. It is a reason to floss consistently every day until the inflammation resolves. As the plaque is removed regularly, the gum inflammation decreases, and the bleeding stops. This process typically takes one to two weeks of consistent daily flossing in mild cases, or two to four weeks in more inflamed gums.
Incorrect Flossing Technique
Snapping floss sharply down between teeth, or pulling it aggressively across the gumline, can mechanically traumatise gum tissue and cause bleeding that is technique-related rather than disease-related. This is less common than inflammation-driven bleeding but worth noting — particularly for patients who are new to flossing or who use a very forceful approach.
Correct flossing technique involves gently guiding the floss between teeth using a back-and-forth sawing motion, then curving it into a C-shape around each tooth and sliding it gently beneath the gumline before moving to the next contact point. It should feel like a gentle hug around the tooth, not a saw through the gum.
Medications and Systemic Factors
Certain medications increase the tendency of gum tissue to bleed — most notably blood thinners such as warfarin, aspirin, and the newer anticoagulants, as well as some antihypertensives and anticonvulsants that cause gum overgrowth. Hormonal changes during pregnancy increase gum sensitivity and inflammatory response, making pregnancy gingivitis a recognised and common condition. Diabetes affects immune response and tissue healing, making diabetic patients significantly more susceptible to gum inflammation and disease.
If you are taking any of these medications, or if you have a systemic condition that affects immune function, bleeding gums warrants a dental assessment — not only to manage the gum condition itself but to ensure the treating dentist is aware of your medical history before any clinical intervention.
When Bleeding Gums Become Something More Serious
Gingivitis — if left untreated — does not stay as gingivitis. It progresses. As bacterial plaque and tartar continue to accumulate and the inflammatory response deepens, the infection spreads below the gumline and begins to destroy the bone and connective tissue that hold the tooth in place. This advanced stage is called periodontitis — and unlike gingivitis, the bone loss it causes is not reversible.
This progression is typically silent. Periodontitis does not usually cause significant pain in its early and moderate stages. Patients often discover they have significant bone loss only at a dental X-ray or a periodontal probing assessment — by which point the condition has been active, and destructive, for some time.
Gum disease is the leading cause of tooth loss in adults worldwide. Not decay. Not trauma. Periodontal disease — which begins as bleeding gums and advances over years of accumulated neglect into bone loss, recession, mobility, and eventually tooth loss. Understanding this makes bleeding gums a more urgent signal than most patients initially treat it as.
Signs That Warrant an Immediate Dental Assessment
The following signs indicate gum disease has progressed beyond simple gingivitis and requires professional evaluation without delay:
- Persistent bleeding that continues despite two to four weeks of consistent, correct flossing and brushing
- Gum recession — the gumline visibly pulling away from teeth, making them appear longer
- Sensitivity at the gumline — particularly to cold, which can indicate exposed root surface
- Bad breath that does not resolve with brushing — a sign of bacterial activity in the gum pockets
- Swelling or pus around the gumline — indicating active infection
- Tooth mobility — any movement in teeth that were previously stable
- Changes in bite — teeth feeling different when biting, which can indicate bone loss altering tooth position
Any of these signs alongside bleeding gums should prompt a dental check-up and a periodontal assessment. The earlier gum disease is identified and treated, the more of the supporting bone and tissue can be preserved.
| Stage | Condition | What Is Happening | Reversible? | Treatment Required |
| Early | Gingivitis | Gum inflammation from plaque — no bone loss | ✅ Fully reversible | Improved home care + professional clean |
| Moderate | Early Periodontitis | Infection spreading below gumline, early bone loss begins | ⚠️ Bone loss is permanent but progression can be halted | Deep cleaning (scaling & root planing) + review |
| Advanced | Moderate Periodontitis | Significant bone loss, recession, possible mobility | ❌ Not reversible — managed, not cured | Periodontal surgery may be required |
| Severe | Advanced Periodontitis | Severe bone loss, tooth mobility, tooth loss risk | ❌ Not reversible | Surgical intervention, possible extraction |
What to Actually Do If Your Gums Bleed When You Floss
This is the practical part — and it is more straightforward than most people expect.
Do Not Stop Flossing
This is the single most important point. Stopping flossing because your gums bleed is the opposite of what your gums need. The bleeding is caused by inflammation, which is caused by plaque, which accumulates precisely in the contact areas between teeth that only floss can reach. Stopping flossing removes the one tool that cleans where the problem is. The gum inflammation will worsen, not improve.
Floss every day. Gently, with correct technique, but consistently. If the bleeding is caused by inflammation rather than an incorrect technique, it will reduce noticeably within one to two weeks and should resolve within a month of consistent flossing.
Improve Your Brushing Technique
Most people brush adequately across the flat surfaces of teeth but miss the gumline — the exact area where plaque needs to be removed most effectively. A soft-bristled toothbrush angled at 45 degrees to the gumline, used with small circular or gentle back-and-forth motions, is the standard recommendation for thorough gumline plaque removal. Electric toothbrushes with oscillating heads are consistently more effective at plaque removal than manual brushes for most patients.
Brush for a full two minutes — twice a day. Most people brush for under a minute, and most of that time is spent on the same familiar surfaces. Use a timer or an electric brush with a built-in timer if you are uncertain.
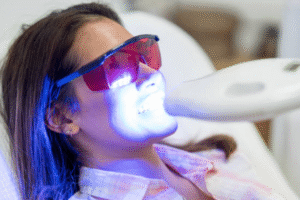
Get a Professional Clean
If you have not had a professional scale and polish in the past six months — or if you have never had one — this is the most impactful single intervention you can make for bleeding gums. Tartar is sustaining the inflammation that flossing alone cannot resolve. A professional clean removes the tartar, gives the gums a clean surface to heal against, and allows the improved home care you put in place to actually work.
At Nova Dental Hospital, a professional clean also includes an assessment of the depth of the gum pockets around each tooth — the key clinical measurement that distinguishes gingivitis from early periodontitis and determines what level of treatment is required.
Book a Periodontal Assessment If Bleeding Persists
If your gums are still bleeding after four weeks of consistent daily flossing, proper brushing, and a professional clean, the problem has moved beyond simple gingivitis and needs a proper clinical evaluation. A periodontal assessment at Nova Dental Hospital measures the depth of the pockets around each tooth, checks for bone loss on X-ray, and gives your dentist the information needed to determine whether gum disease treatment beyond a standard clean is required.
✅ Quick Tip: The Right Flossing Technique
- Use approximately 40–45 cm of floss, winding most of it around your middle fingers so you have a clean section for each gap.
- Guide the floss between teeth with a gentle sawing motion — never snap it down sharply onto the gum.
- Curve the floss into a C-shape around each tooth and slide it gently 1–2 mm beneath the gumline — this is where plaque accumulates.
- Use a fresh section of floss for each tooth contact. Moving the same section of floss from gap to gap redistributes the bacteria you just removed.
- Floss interdental brushes are an excellent alternative for patients with larger gaps between teeth or fixed orthodontic appliances — they remove plaque from around brackets and wires effectively.
Common Misconceptions About Bleeding Gums
“My gums always bleed — it must just be normal for me.”
This is the most common and most consequential misconception. Habitual bleeding is not a personal baseline — it is habitual inflammation. The fact that it has been happening for years does not make it normal; it means the underlying cause has been present and unaddressed for years. Every patient who has been told by a dentist that their gum disease is more advanced than they expected started out thinking their bleeding was normal.
“Bleeding means I am brushing too hard — I should brush more gently.”
Brushing trauma can cause gum bleeding but it looks different — it is typically localised to specific areas where technique is poor, and the gum tissue shows signs of physical wear rather than generalised redness and swelling. Inflammation-driven bleeding, which accounts for the vast majority of cases, is not caused by brushing pressure. Switching to a soft-bristled brush and refining your technique is sensible, but reducing brushing pressure will not resolve bleeding caused by inflammation.
“I use mouthwash every day, so my gums should be fine.”
Mouthwash is an adjunct to mechanical cleaning — not a substitute for it. Antibacterial mouthwashes can reduce the bacterial load in the mouth, which is helpful, but they cannot remove plaque or tartar from the tooth surface. The physical disruption of plaque by brushing and flossing is what prevents and resolves gum inflammation. A patient who uses mouthwash twice a day but does not floss will still develop tartar in the contact areas between teeth and still develop gingivitis.
“The dentist can sort it out when I go — I will deal with it then.”
This is the reasoning that allows gingivitis to progress to periodontitis. A professional clean can reset the gum environment and remove existing tartar, but it cannot reverse bone loss that has already occurred. The daily maintenance between dental visits — the brushing, the flossing, the consistent plaque removal — is what prevents the condition from advancing. The dentist’s role is to clean what home care cannot reach and to monitor for progression. The patient’s daily routine is the primary treatment.
The Link Between Gum Health and Your General Health
This section is worth reading even for patients who are not particularly concerned about their gums — because the relationship between gum disease and systemic health is one of the most clinically significant and least publicly known connections in medicine.
Research consistently demonstrates links between chronic periodontal disease and a range of systemic conditions including:
- Cardiovascular disease — chronic gum inflammation contributes to systemic inflammatory load, and the bacteria involved in periodontal disease have been found in arterial plaque
- Diabetes — the relationship is bidirectional: uncontrolled diabetes worsens gum disease, and poorly controlled gum disease worsens glycaemic control
- Adverse pregnancy outcomes — periodontal disease during pregnancy is associated with increased risk of preterm birth and low birth weight
- Respiratory conditions — aspiration of oral bacteria has been linked to pneumonia and chronic obstructive pulmonary disease in susceptible individuals
- Cognitive decline — emerging research suggests associations between periodontal bacteria and Alzheimer’s disease, though the causal relationship is still being established
The mouth is not a separate system from the rest of the body. Chronic infection and inflammation in the gum tissue enter the bloodstream and exert effects that extend well beyond the teeth. Treating gum disease is not merely a dental matter — it is a health matter.
Frequently Asked Questions
FAQ 1: How long does it take for gum bleeding to stop once I start flossing regularly?
For most patients with mild gingivitis and no significant tartar buildup, consistent daily flossing and brushing will produce a noticeable reduction in bleeding within one to two weeks, and the bleeding should resolve within three to four weeks. If you also have a professional clean during this period — which removes the hardened tartar that home care cannot — the resolution tends to be faster. If bleeding continues beyond four weeks of genuinely consistent home care and a professional clean, it is time for a periodontal assessment to rule out deeper gum disease.
FAQ 2: Can gum bleeding be caused by something other than gum disease?
Yes, though gum disease and tartar-driven inflammation account for the large majority of cases. Other causes include blood-thinning medications, vitamin C or vitamin K deficiency, hormonal changes during pregnancy or the menstrual cycle, certain medical conditions affecting clotting or immune response, and in rare cases, leukaemia or other blood disorders. If your gums bleed heavily and persistently despite good oral hygiene, or if bleeding occurs elsewhere in the body alongside gum bleeding, a medical assessment alongside a dental evaluation is warranted.
FAQ 3: My dentist said I have gum disease but my gums do not hurt — how is that possible?
Gum disease is famously painless in its early and moderate stages. Gingivitis causes inflammation but rarely pain. Early and moderate periodontitis causes bone loss that the patient does not feel until the damage is substantial. This is why it progresses so far before most patients are aware of it, and why regular dental check-ups are essential — the probing assessment and X-rays that identify gum disease are the only reliable way to catch it before irreversible damage has occurred. If you have been told you have gum disease, the treatment options at Nova Dental Hospital range from a deep clean for early-stage disease to more advanced periodontal therapy for established bone loss.
FAQ 4: Is it safe to floss if my gums are already swollen and bleeding?
Yes — and it is important that you do. Swollen, bleeding gums are inflamed gums, and the inflammation is sustained by the plaque that flossing removes. Avoiding flossing because the gums are sensitive or bleed easily allows the plaque to continue accumulating and the inflammation to worsen. Floss gently, use the correct technique, and expect the discomfort and bleeding to reduce over one to two weeks as the inflammation resolves. If swelling is severe, or if there is visible pus or significant pain, see a dentist before continuing home care — these signs indicate an active infection that needs clinical management.
FAQ 5: How often should I be visiting a dentist to keep my gums healthy?
For most adults with healthy or well-managed gums, a dental check-up and professional clean every six months is the standard recommendation. For patients with a history of gum disease, active periodontitis, or high plaque accumulation rates, more frequent visits — every three to four months — are typically recommended to maintain the gains made from treatment and catch any recurrence early. If you are in Gandhinagar and have not had a check-up recently, a general dentistry consultation at Nova Dental Hospital includes a full gum assessment and will tell you exactly where your gum health stands and what, if anything, needs attention. Patients who have had treatment with us are also welcome to leave a review on our Google Business Profile.
🔑 Key Takeaways
- Gums bleeding when flossing is not normal — it is a sign of gum inflammation, almost always caused by plaque and tartar at the gumline.
- The most common cause is gingivitis, which is fully reversible with consistent home care and a professional clean.
- Do not stop flossing because of bleeding — flossing removes the plaque that is causing the bleeding. Stopping makes the problem worse.
- If bleeding persists beyond four weeks of proper home care and a professional clean, a periodontal assessment is needed.
- Gingivitis that is left untreated progresses to periodontitis — irreversible bone loss that is the leading cause of tooth loss in adults.
- Gum health is not isolated to the mouth — chronic gum disease is linked to cardiovascular disease, diabetes, and adverse pregnancy outcomes.
- Regular six-monthly check-ups are the most reliable way to catch gum disease before it becomes advanced.
Conclusion: Bleeding Gums Are a Signal, Not a Sentence
If your gums bleed every time you floss, you now know what that means, what causes it, and what to do about it. The good news is that in most cases — particularly for patients with gingivitis rather than established periodontitis — the solution is genuinely within reach. Better flossing technique, consistent daily home care, and a professional clean to remove the tartar that home care cannot is enough to resolve the problem for the majority of patients.
The key is not to normalise it, not to avoid flossing, and not to wait until other symptoms appear before taking it seriously. Bleeding gums are early — which means they are easy to treat. The same condition left for years becomes significantly harder to manage and leads to damage that cannot be undone.
At Nova Dental Hospital in Gandhinagar, a gum assessment is part of every clinical check-up. If you have noticed bleeding gums, recurring bad breath, or any of the other signs discussed in this blog, a consultation with our team will give you a clear picture of where your gum health stands — and a straightforward plan to improve it.