What Are the Signs and Symptoms of a Tooth Infection?
What Are the Signs and Symptoms of a Tooth Infection?
A tooth infection, also called a dental abscess, is a serious condition that requires prompt professional attention. Understanding tooth infection symptoms helps you recognize when you need urgent dental care and prevents complications that can threaten not only your oral health but your overall wellbeing. While tooth pain is the most obvious sign, infections present with various symptoms that shouldn’t be ignored, and knowing what to watch for empowers you to seek timely treatment.
At Nova Dental Hospital in Gandhinagar, we provide emergency dental care for patients near PDPU and Gift City experiencing dental infections and other urgent conditions. Recognizing tooth infection symptoms early allows intervention before the infection spreads, potentially causing serious health complications. Whether you’re experiencing dental pain or suspect something isn’t right, understanding the signs of tooth abscess and when to seek emergency care can make a crucial difference in protecting your oral health and preventing dangerous complications.
What Is a Tooth Infection and How Does It Develop?
Before discussing specific tooth infection symptoms, understanding what causes these infections and how they progress helps you appreciate why prompt treatment is essential for your oral health.
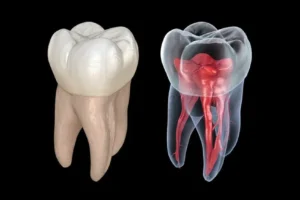
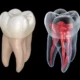
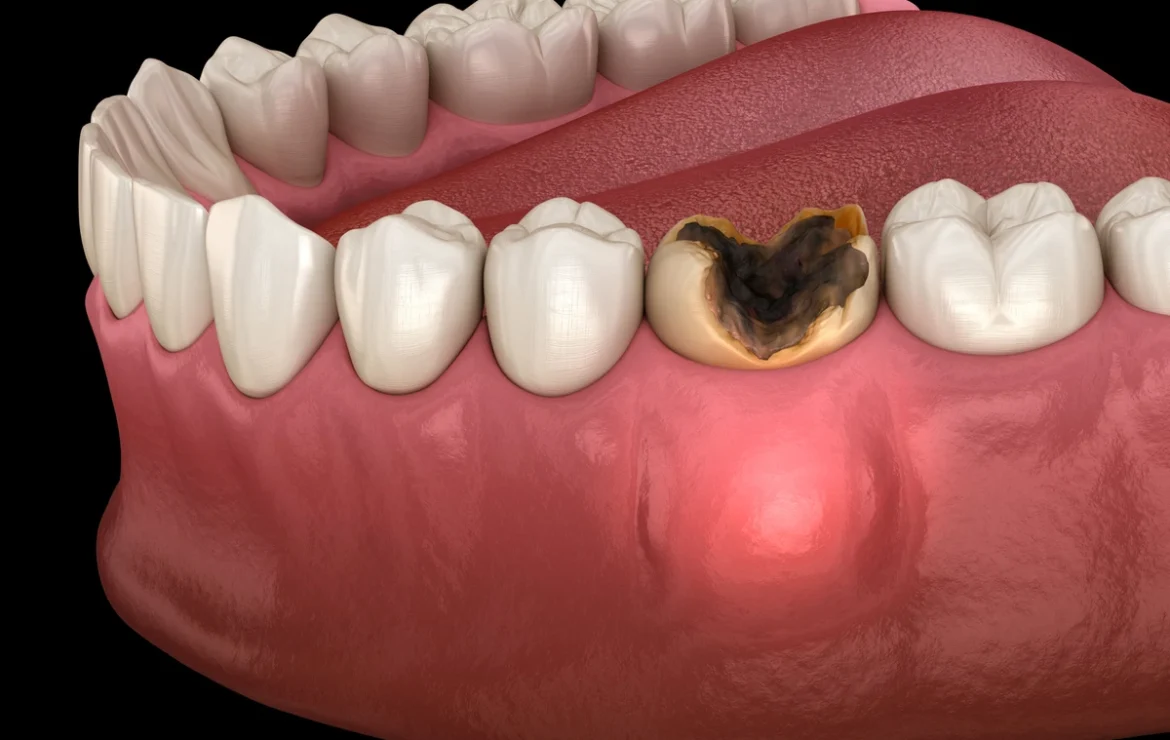
A tooth infection occurs when bacteria invade the innermost part of your tooth, called the pulp, which contains nerves, blood vessels, and connective tissue. This invasion typically happens in one of several ways. Untreated tooth decay is the most common cause—when a cavity penetrates through the protective enamel and dentin layers, bacteria reach the pulp chamber. The body’s immune system cannot effectively fight infection in this enclosed space, allowing bacteria to thrive and eventually kill the pulp tissue.
Dental trauma from injuries, accidents, or even aggressive dental work can crack or chip teeth, creating pathways for bacteria to enter. Sometimes trauma doesn’t immediately cause infection but damages the tooth’s blood supply, eventually leading to pulp death and subsequent infection. A tooth abscess can develop months or even years after an injury that seemed to heal without complications.
Gum disease that progresses deeply can allow bacteria to access tooth roots through periodontal pockets. This type of infection, called a periodontal abscess, forms in the gum tissue around the tooth rather than inside the tooth itself, though it produces similar symptoms and requires urgent treatment.
Failed dental work, such as deep fillings that didn’t adequately remove all decay, or cracked old restorations that allow bacterial leakage, can lead to infections developing beneath crowns or fillings. These situations are particularly frustrating because the tooth was previously treated, but incomplete decay removal or compromised restoration integrity allows bacteria to access the pulp.
Once bacteria establish infection in the pulp chamber, the confined space prevents drainage. Pus accumulates, creating pressure that causes the characteristic severe pain of tooth abscess. If the infection isn’t treated, it can erode through the bone at the tip of the tooth root, forming an abscess pocket in the surrounding bone and potentially spreading to other areas.
Common Tooth Infection Symptoms You Shouldn’t Ignore
Recognizing tooth infection symptoms promptly allows you to seek treatment before complications develop. While symptoms vary in severity and presentation, certain signs consistently indicate infection requiring professional dental care.
Severe, persistent toothache represents the hallmark tooth infection symptom. This pain often throbs and intensifies over time rather than coming and going like sensitivity. The discomfort may feel sharp and shooting or deep and aching. Unlike sensitivity to specific triggers, infection pain is often constant, though it may worsen with pressure, heat, or when lying down. The pain from a tooth abscess can be so intense it interferes with sleep, eating, and normal activities.
Sensitivity to hot and cold temperatures, particularly when sensitivity to heat is prolonged and painful, suggests infection. While cold sensitivity is common with various dental issues, persistent sensitivity to hot foods and beverages that continues after the stimulus is removed often indicates nerve damage from infection. Some patients report that cold temporarily relieves pain from infection by numbing the area, while heat intensifies discomfort.
Swelling in your face, jaw, or lymph nodes signals that infection is spreading beyond the tooth. Facial swelling can range from barely noticeable puffiness to dramatic, alarming enlargement that distorts your appearance. Swollen lymph nodes in your neck, particularly under the jaw, indicate your immune system is fighting infection. Any facial swelling associated with dental pain warrants immediate evaluation by an emergency dentist, as spreading infection can become dangerous quickly.
Tender, swollen, or bleeding gums around the affected tooth often accompany dental infection Gandhinagar dentists diagnose. The gums may appear red and inflamed, feel soft and swollen, or develop a pimple-like bump called a fistula through which the abscess drains. If you notice a recurring bump on your gums that occasionally releases a salty, unpleasant-tasting fluid, this represents the body’s attempt to drain infection and requires professional treatment.
Persistent foul taste in your mouth or bad breath that doesn’t improve with brushing may result from draining infection. The bacteria causing tooth abscess produce waste products and toxins that create distinctly unpleasant odors and tastes. While bad breath has many causes, when it accompanies other tooth infection symptoms, infection is likely contributing.
Difficulty opening your mouth, also called trismus, can develop when infection causes muscle spasm or inflammation in the jaw area. This symptom suggests infection is affecting surrounding tissues and structures beyond the tooth itself. Limited mouth opening makes eating difficult and indicates the infection requires immediate attention.
Recognizing Severe Tooth Infection Symptoms Requiring Emergency Care
While all tooth infections need professional treatment, certain tooth infection symptoms indicate dangerous complications requiring immediate emergency dental care. Understanding when a situation becomes urgent helps you make appropriate decisions about seeking care.
High fever, typically 101°F or above, accompanying dental pain signals that infection has spread systemically. Fever indicates your body is mounting an immune response to bacteria that have entered your bloodstream. This situation requires urgent medical attention, as untreated dental infections can lead to sepsis, a life-threatening condition. Don’t wait to see if fever resolves on its own—seek emergency care immediately.
Difficulty breathing or swallowing represents a medical emergency. When infection spreads to spaces in the neck and throat, it can cause swelling that compromises your airway. These symptoms require immediate emergency room care, not just dental treatment, as they can rapidly become life-threatening. Difficulty swallowing or a sensation that your throat is closing warrants calling emergency services without delay.
Severe facial swelling that rapidly worsens or affects your eye or causes vision changes indicates aggressive infection spread. Dental infections can spread to the spaces around the eye and into the skull, creating dangerous complications. Any visual changes, severe headaches, or swelling that closes your eye requires immediate emergency evaluation.
Rapid heart rate, dizziness, confusion, or extreme fatigue suggests possible sepsis from spreading infection. These systemic symptoms indicate bacteria have entered your bloodstream, triggering a whole-body inflammatory response. Sepsis is a medical emergency requiring hospitalization, not just dental treatment. If dental pain is accompanied by these concerning systemic symptoms, go to an emergency room immediately.
Dehydration resulting from inability to eat or drink due to severe pain or swelling requires urgent attention. While perhaps not immediately life-threatening like breathing difficulty, severe dehydration complicates infection and delays healing. If you haven’t been able to consume adequate fluids for 24 hours due to dental problems, seek emergency care.
Less Obvious Tooth Infection Symptoms That Still Need Attention
Not all tooth infections present with dramatic, obvious symptoms. Some tooth abscess cases develop more subtly, making recognition challenging. However, these quieter presentations still require professional treatment to prevent progression.
Dull, persistent ache in your tooth, jaw, or ear that doesn’t resolve after several days may indicate developing infection. Some infections cause less intense pain than others, particularly if the tooth’s nerve has already died. This dull discomfort might seem manageable, leading patients to delay seeking care. However, absence of severe pain doesn’t mean absence of infection—bacteria continue damaging bone and surrounding tissues even when pain is moderate.
Tooth discoloration, particularly darkening to gray or brown, can signal that the tooth’s nerve has died, often due to infection or trauma. The color change results from breakdown products from dying nerve tissue being absorbed into the tooth structure. A darkened tooth needs evaluation even without pain, as infection may be present without causing discomfort if the nerve is no longer vital.
Loosening of a tooth that was previously stable sometimes accompanies chronic infection. As bacteria destroy bone supporting the tooth, it begins to feel mobile. This symptom typically develops in long-standing infections rather than acute cases. Even without severe pain, a tooth that’s becoming loose requires prompt evaluation to determine the cause and appropriate treatment.
Recurring pimple-like bump on the gums, called a sinus tract or fistula, represents the body’s attempt to drain infection. The bump may appear, drain fluid with a bad taste, temporarily disappear, then return cyclically. While drainage provides some pressure relief, it doesn’t eliminate the underlying infection. This finding always indicates the need for professional treatment to address the source of infection.
Increased tooth sensitivity when biting or chewing, even without spontaneous pain, can indicate infection affecting the periodontal ligament around the tooth root. Pressure sensitivity that develops or worsens over time warrants evaluation to rule out infection or other problems requiring treatment.
How Tooth Infection Symptoms Differ From Other Dental Problems
Many dental conditions cause pain and discomfort, making it sometimes challenging to distinguish tooth infection symptoms from other issues. Understanding these differences helps you communicate effectively with your dentist and understand the urgency of your situation.
Tooth sensitivity from exposed roots or enamel erosion causes brief, sharp pain in response to specific triggers like cold, heat, or sweet foods. This pain subsides quickly when the stimulus is removed. In contrast, pain from tooth abscess is typically more constant, throbbing, and persists regardless of triggers. Sensitivity rarely causes swelling or fever, which are common with infection.
Cracked teeth produce sharp pain when biting, particularly when releasing pressure. The pain from cracks is highly specific to mechanical stress, while infection pain is more generalized and constant. Cracks don’t typically cause facial swelling or fever, though they can eventually lead to infection if bacteria enter through the crack.
Sinus infections can cause upper tooth pain that mimics dental infection, as the roots of upper back teeth extend into the sinus cavity. However, sinus-related tooth pain typically affects multiple teeth on one side rather than a single tooth. It’s often accompanied by sinus congestion, nasal discharge, and facial pressure across the cheeks and under the eyes. Movement and position changes affect sinus pain more than dental infection pain.
TMJ disorders causing jaw pain differ from tooth infection symptoms because TMJ pain centers around the jaw joint, affects both sides, and is associated with clicking or popping sounds when moving the jaw. TMJ issues don’t cause tooth-specific pain, swelling inside the mouth, or fever.
Gum disease causes symptoms like bleeding, swelling, and bad breath but typically affects broader areas rather than being localized to one tooth. Periodontal disease develops gradually over time, while tooth abscess often produces more acute, severe symptoms. However, advanced gum disease can lead to abscesses, so these conditions sometimes overlap.
What Happens If Tooth Infection Symptoms Are Ignored?
Understanding the potential consequences of untreated tooth infections underscores the importance of seeking prompt care when you recognize tooth infection symptoms. The complications of dental infection Gandhinagar patients risk by delaying treatment range from uncomfortable to life-threatening.
The infection continues spreading through bone and soft tissue if left untreated. What begins as infection confined to one tooth can erode through jawbone, spread into adjacent teeth, and extend into facial tissues. This progression causes increasingly severe pain, swelling, and visible deformity that becomes more difficult to treat the longer it continues.
Tooth abscess can create a fistula or drainage pathway through the gum tissue, sometimes providing temporary relief as pressure decreases. However, this doesn’t resolve the infection—it simply provides an outlet for drainage. The underlying infection persists, continues damaging tissue, and may spread despite the presence of a draining fistula.
Chronic dental infections severely compromise your oral health, destroying significant amounts of jawbone and potentially requiring extensive reconstruction after the infection is finally treated. Bones adjacent to long-standing infections experience substantial loss that affects stability of multiple teeth and can alter facial structure.
Systemic spread of dental infection can lead to serious, potentially life-threatening complications. Bacteria from tooth abscess can spread through bloodstream to heart, brain, lungs, or other organs. Endocarditis (heart infection), brain abscesses, and pneumonia can all result from untreated dental infections. People with compromised immune systems, heart conditions, or artificial joints face particularly high risks from dental infection spread.
Ludwig’s angina, a severe infection affecting floor of the mouth and neck, can develop from untreated lower tooth abscess. This condition causes rapidly progressing swelling that can block airways, creating a medical emergency. While relatively rare, Ludwig’s angina demonstrates the serious potential consequences of neglected dental infections.
Sepsis, the body’s extreme response to infection, can result from dental infection bacteria entering the bloodstream. Sepsis triggers widespread inflammation affecting multiple organ systems and can progress to septic shock, a life-threatening condition with high mortality rates. Dental infections causing sepsis require hospitalization with intravenous antibiotics and intensive medical care.
Death from dental infections, while uncommon in modern times, still occurs when infections go untreated and spread aggressively. These tragic outcomes are preventable with prompt dental care when tooth infection symptoms appear.
Diagnosis and Treatment of Tooth Infections
When you visit Nova Dental Hospital with tooth infection symptoms, comprehensive evaluation identifies the source and extent of infection, guiding appropriate treatment to resolve the problem and prevent complications.
Your dentist begins with detailed examination of the affected tooth and surrounding tissues, looking for swelling, tenderness, discoloration, or drainage. They gently tap teeth to assess sensitivity and check for looseness indicating bone loss. Your medical history helps identify risk factors and guide treatment decisions.
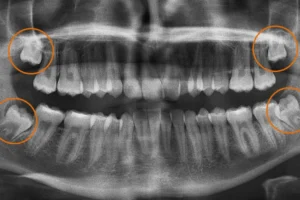
Dental X-rays reveal infection that isn’t visible during clinical examination. Radiographs show bone loss at tooth roots, abscesses in surrounding bone, and other signs of infection. These images help your dentist determine infection extent and plan appropriate treatment. In some cases, additional imaging like CT scans provides three-dimensional views of complex infections.
Treatment for tooth abscess focuses on eliminating infection and preserving the tooth when possible. Antibiotics alone don’t cure dental infections because bacteria are sealed inside the tooth where medication cannot reach effectively. While antibiotics help control infection spread and are necessary for certain high-risk patients, definitive treatment requires removing the infection source.
Root canal therapy saves infected teeth by removing diseased pulp tissue from inside the tooth, thoroughly cleaning and disinfecting the root canal system, then sealing it to prevent reinfection. After root canal treatment, the tooth is typically restored with a crown to protect and strengthen it. Success rates for root canal therapy are high, allowing patients to keep natural teeth despite previous severe infection.
Tooth extraction becomes necessary when infection has destroyed so much tooth structure that restoration isn’t feasible, or when bone loss is too extensive to support the tooth. While extraction resolves the immediate infection, planning for tooth replacement with implants, bridges, or dentures becomes important for maintaining function and preventing adjacent teeth from shifting.
Incision and drainage may be necessary for abscesses that have formed pockets of pus in surrounding tissues. This procedure provides immediate pressure relief and allows the body to fight infection more effectively while definitive treatment addresses the tooth itself.
Preventing Tooth Infections Through Good Oral Health
While understanding tooth infection symptoms helps you recognize when problems develop, preventing infections in the first place protects your oral health more effectively. These practices minimize your risk of developing tooth abscess.
Maintain excellent oral hygiene through thorough brushing twice daily and daily flossing. These fundamental practices remove plaque bacteria before they cause cavities that can lead to infections. Use fluoride toothpaste to strengthen enamel and make teeth more resistant to decay. While basic advice, consistent home care is genuinely your best defense against dental infections.
Schedule regular dental checkups and professional cleanings, typically every six months. These appointments allow early detection of cavities, cracks, and other problems before they progress to infection. Professional cleanings remove tartar buildup that home care misses and helps prevent gum disease that can lead to abscesses. Early treatment of small cavities prevents the deep decay that eventually reaches tooth pulp and causes infection.
Address dental problems promptly when they develop. If you notice new tooth pain, sensitivity, or other changes, schedule evaluation rather than hoping symptoms resolve on their own. Early intervention treats problems with simpler procedures, whereas delayed treatment often means more extensive work is needed. Cavities, cracks, and other issues don’t improve without treatment and often worsen over time.
Protect teeth from trauma by wearing mouthguards during sports and avoiding using teeth as tools to open packages or crack nuts. Trauma that cracks or damages teeth creates pathways for bacteria and can damage blood supply to the pulp, eventually leading to infection.
Maintain good overall health and manage chronic conditions like diabetes that increase infection risk. Elevated blood sugar impairs immune function and wound healing, making dental infections more likely and more difficult to control. Work with your physician to keep chronic conditions well-controlled, protecting both your general and oral health.
Avoid tobacco use, which dramatically increases risk of gum disease and impairs healing from dental procedures. Smokers develop more frequent and severe dental infections compared to non-smokers and respond less well to treatment.
Conclusion: Recognizing and Addressing Tooth Infection Symptoms
Understanding tooth infection symptoms empowers you to recognize when dental problems require urgent attention and seek appropriate care before complications develop. While some tooth pain represents minor issues that can wait for regular appointment scheduling, the signs of tooth abscess warrant prompt evaluation and treatment to prevent infection spread and potentially serious consequences.
At Nova Dental Hospital in Gandhinagar, Dr. Happy Patel and our experienced team provide comprehensive care for dental infections, from emergency treatment of acute abscesses to preventive care that minimizes infection risk. We serve patients near PDPU and Gift City with urgent dental care when needed and ongoing support for maintaining optimal oral health.
If you’re experiencing tooth infection symptoms including persistent toothache, facial swelling, fever, or other concerning signs, don’t delay seeking care. Contact us immediately for emergency evaluation. Prompt treatment resolves infection, eliminates pain, and prevents dangerous complications from developing. Your oral health and overall wellbeing are too important to risk by ignoring warning signs of dental infection.
Remember that prevention through excellent oral hygiene and regular dental care remains your best defense against tooth infections. However, when problems do develop despite your best efforts, recognizing tooth infection symptoms and seeking timely professional care makes all the difference in protecting your health and preserving your natural teeth.
Frequently Asked Questions
Can a tooth infection go away on its own without treatment?
No, tooth infections never resolve without professional treatment. While symptoms might temporarily seem to improve, particularly if a fistula forms allowing the abscess to drain, the underlying infection persists and continues damaging tissue. Bacteria sealed inside the tooth or bone require mechanical removal through root canal therapy or extraction. Antibiotics alone don’t cure dental infections because medication cannot reach bacteria protected inside the tooth structure. Untreated tooth abscess inevitably worsens, potentially spreading to dangerous areas. If you suspect infection based on tooth infection symptoms, seek prompt dental care rather than hoping it will resolve independently.
How quickly do tooth infection symptoms develop?
Development speed varies considerably. Some tooth infections cause sudden, severe pain that develops over hours to days, while others progress slowly over weeks or months with gradually worsening symptoms. Infections following acute trauma or in teeth with previous large fillings often cause rapid symptom onset. Conversely, infections in teeth where the nerve is slowly dying from chronic decay may develop insidiously with minimal pain until the infection spreads beyond the tooth. Regardless of symptom progression speed, all dental infections require professional treatment. Don’t dismiss slowly developing symptoms as less serious—chronic infections can cause extensive damage while causing less dramatic discomfort than acute cases.
Are tooth infections contagious?
Tooth infections themselves aren’t contagious—you can’t “catch” a dental abscess from someone else. However, the bacteria that cause tooth infections can be transmitted through saliva, particularly Streptococcus mutans, which contributes to cavity formation. Sharing utensils, kissing, or other activities involving saliva exchange can transfer bacteria, though this doesn’t directly cause infections in healthy teeth. Good oral hygiene and regular dental care protect against infection regardless of bacterial exposure. If you have a tooth infection, focus on getting treatment rather than worrying about transmission, though maintaining good hygiene practices benefits everyone’s oral health.
Can I wait until morning if I notice tooth infection symptoms at night?
This depends on symptom severity. Mild to moderate tooth pain without facial swelling, fever, or difficulty breathing can typically wait until morning or the next business day for evaluation at a dental clinic Gandhinagar. However, seek immediate emergency care for severe symptoms including high fever, significant facial swelling, difficulty breathing or swallowing, or signs of systemic illness. These serious tooth infection symptoms indicate dangerous infection spread requiring urgent intervention. When unsure, err on the side of caution—call your emergency dentist for guidance, or go to an emergency room if potentially serious symptoms are present. Dental emergencies can deteriorate rapidly, making timely care crucial.
Will antibiotics cure my tooth infection without other treatment?
Antibiotics alone cannot cure tooth infections. While these medications help control bacterial spread and are essential for patients with certain health conditions or severe infections, they don’t eliminate bacteria sealed inside the tooth structure. Antibiotics may provide temporary symptom relief, but infection returns once medication is discontinued unless the source is mechanically removed through root canal therapy or extraction. Think of antibiotics as supportive treatment that controls infection while allowing safe performance of definitive procedures. Don’t skip dental treatment hoping antibiotics will suffice—they’re just one component of comprehensive care for tooth abscess.